Contaminated food and water infected nearly 20,000 people in 2023 : Revista Pesquisa Fapesp

Nausea and vomiting can be signs of something other than dengue fever, the current major health concern. Similarly, stomach pain and diarrhea aren’t necessarily the result of a bad meal and nothing else. They may also be symptoms of illnesses caused by microorganisms carried in contaminated water or poorly washed or undercooked food—a long-standing problem that still persists in Brazil.
Between 2000 and 2021, Brazil’s Ministry of Health recorded 375,258 cases of what are known as food- and water-borne diseases (FWBD), caused by 78 different organisms, such as bacteria, viruses, worms, and protozoa. In 2023 alone, 19,671 people contracted diseases caused by contaminated water or food in Brazil, of which 31 died. That was more than in the previous year, which saw 14,336 cases and 10 deaths.
The conclusions are based on data from the federal government’s Information System for Notifiable Illnesses and Injuries (SINAN), analyzed by researchers from the Community University of Chapecó (Unochapecó) in Santa Catarina and the Federal University of Santa Maria (UFSM) in Rio Grande do Sul. Their results were published in an article in the Journal of Water and Health in June.

UN Photo / Sophia ParisChildren wash their hands in a river contaminated with cholera bacilli in the village of Jurve, HaitiUN Photo / Sophia Paris
Records from SINAN indicate that at times, hundreds of children in daycare centers or schools contract diarrhea, though they usually receive treatment and recover. The mortality rate is high, however, in institutions for the elderly. In March 2023, 43 residents of a nursing home in Cataguases, Minas Gerais, came down with severe diarrhea after eating vegetables contaminated with rotavirus. All of them died. In July this year, another 23 people at a nursing home in Rio de Janeiro died after being infected with norovirus, which also causes diarrhea, vomiting, and a high fever. People with weakened immune systems, the elderly, young children, pregnant women, and infants are the most vulnerable groups.
Improvements in sanitation infrastructure—water, sewage, and waste collection—have likely contributed to a gradual decline in the number of cases and deaths each year. Even so, only 84.9% of the Brazilian population currently has access to potable water, according to 2022 data from the National Sanitation Information System (SNIS). That means that in 2022, 33 million people did not have access to clean water. Even fewer had access to sewage treatment, at just 44.5%, meaning most household waste was still being dumped untreated into rivers, potentially contaminating them with disease-causing microorganisms.
In more remote areas, cisterns of filtered and chlorinated water are used to reduce waterborne diseases. A team from the Public Health Agency of Canada interviewed 1,863 people from 377 households with cisterns and 1,816 people from 397 households without them in rural Pernambuco. As described in a February 2013 article in BMC Infectious Diseases, in the 30 days prior to the survey, children aged under five who lived in houses without a cistern suffered from diarrhea at twice the rate of those with a cistern.
The World Health Organization (WHO) lists 250 such diseases caused by bacteria, viruses, intestinal parasites, bacterial and fungal toxins, or chemical substances, such as heavy metals that can be transmitted through water, drinks, dairy products, meat, fish, ice cream, fruit, and vegetables. Contamination can occur at any stage in the food production chain—cultivation, harvesting, processing, storage, transport, handling, or preparation.

Léo Ramos Chaves / Pesquisa FAPESPFood transportation is one of the stages when contamination by disease-causing microorganisms can occurLéo Ramos Chaves / Pesquisa FAPESP
The problem can have a major impact on the population. Between January 2024 and March 2025, for example, 16 countries in southern and eastern Africa recorded more than 178,000 cases of cholera, caused by the bacterium Vibrio cholerae, resulting in approximately 2,900 deaths. In Brazil, after an epidemic that caused 60,000 cases and 1,000 deaths in 1991, cholera has only appeared in isolated cases, in Pernambuco in 2004 and 2005, and in Bahia in April 2024.
The Brazilian Ministry of Health recorded an average of 662 FWBD outbreaks per year from 2007 to 2020. Ubiratan Bones, a sanitary and environmental engineer from Unochapecó and leader of the study published in the Journal of Water and Health, believes the records are incomplete. “Underreporting is still widespread, especially in areas without basic sanitation, where sewage runs in the open, or where healthcare access is limited,” he says. He warns that difficulties accessing medical care often lead to self-medication, which is not recommended.
“Underreporting is related to factors such as the absence of lab diagnoses, failures in reporting systems, ignorance or negligence of mandatory reporting requirements, and a lack of epidemiology resources and expertise,” says Farah Chequer, a pharmaceutical biochemist from the Federal University of São João del-Rei (UFSJ) in Minas Gerais who was not involved in the study. Chequer was one of the authors of a study published in the journal Health and Research in December 2022, also based on data from SINAN, that supports the idea that the reported figures are underestimates.
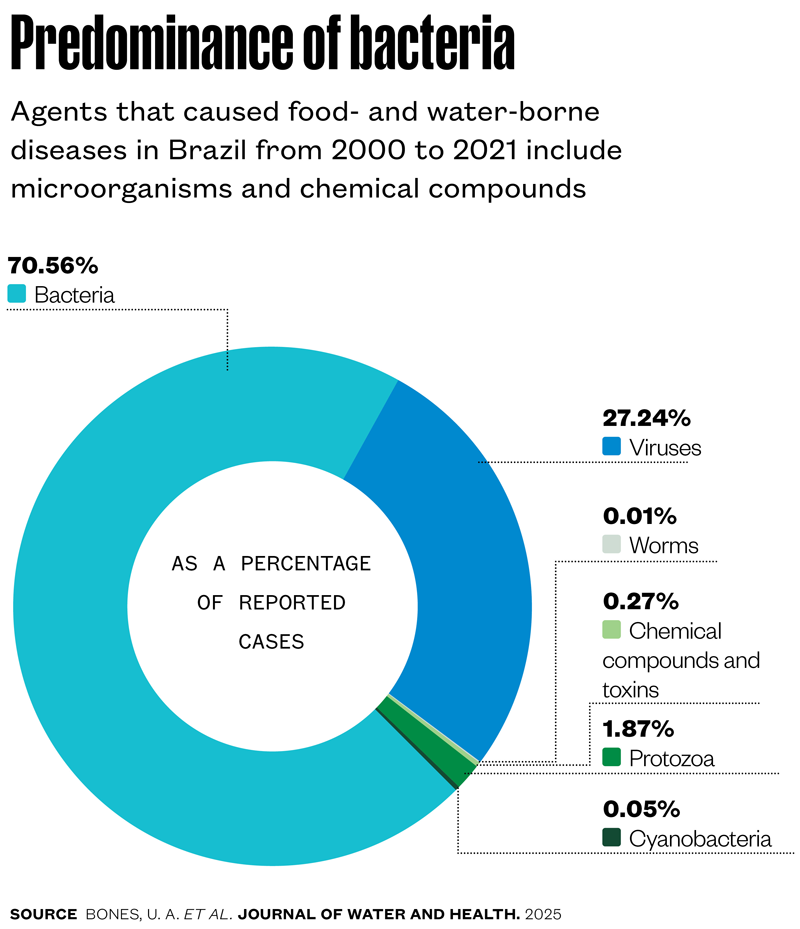
In 1918, in the book Urupês, writer Monteiro Lobato (1882–1948) introduced the character Jeca Tatu, a poor rural man whose lack of energy was not laziness as it first seemed, but the result of an infection by intestinal worms that caused anemia and weakness. Worm infestations were a common concern in Brazil in the early twentieth century. Today, worms like Ancylostoma duodenale and Necator americanus account for just 0.01% of cases recorded in the period of study (see infographic).
Bacteria have dominated as the main agents of food- and water-borne disease in recent decades, responsible for 70% of cases, especially Escherichia coli, which accounts for 30% of cases and causes diarrhea that can be fatal. Other species of bacteria—Bacillus cereus, Clostridium, Salmonella, Shigella, Staphylococcus aureus—are among 10 pathogens responsible for 95% of cases. Viruses, such as hepatitis, and worms, such as roundworm (Ascaris lumbricoides), also make the list. E. coli mainly spreads through water, and Salmonella through food—like the others, most people pick up the infection in their own homes, which is three times more likely than getting it from a restaurant.
In the home, many common habits allow disease-causing organisms to spread. From September 2023 to April 2024, researchers from the University of Vila Velha (UVV) in Espírito Santo and Ohio State University conducted an online questionnaire consisting of 41 questions to survey the food hygiene practices of 1,043 participants. According to the results, published in PLOS ONE in June, 67.3% of participants reported that they did not wash food before storing it in the refrigerator, 64.9% used the same cutting board for meat and raw vegetables, and 52.7% washed vegetables with water alone. Respondents from the North and Central-West regions were at a greater risk of suffering from foodborne illnesses than those from the Southeast. Only 3% said they use a thermometer to check if meat is cooked, which helps prevent the ingestion of infectious pathogens.
Data from SINAN show that infectious agents can strike at any time, in small villages or large cities. In July 2000, 66 people in Gama, Federal District, and 163 in Santa Carmen, Mato Grosso, fell ill with salmonellosis after eating eggs contaminated with Salmonella spp., leading to diarrhea, vomiting, fever, abdominal pain, and in severe cases, dehydration. In August 2000, 594 people at a daycare center in Estância Velha, Rio Grande do Sul, developed shigellosis, caused by food contaminated by the bacteria Shigella sonnei, with symptoms including fever, nausea, and vomiting.
Prevention relies on the same precautions taken in Jeca Tatu’s time: washing hands with soap and water before preparing or eating food, using the bathroom, changing diapers, or handling pets; drinking water that has been filtered, boiled, or treated with sodium hypochlorite (available for free at basic health centers); properly cooking meat, eggs, and seafood; not eating raw or undercooked food; washing fruit and vegetables with treated water or hypochlorite solution; and promptly seeking medical care in cases of vomiting, diarrhea, or abdominal pain. “It never hurts to reinforce the importance of hygiene measures for children and adults, no matter the location,” emphasizes Bones.
The story above was published with the title “Hitching a ride on the water” in issue 355 of September/2025.
Scientific articles
ALEGRANSI BONES, U. et al. Epidemiologic study of waterborne and foodborne diseases in Brazil: Mapping trends and challenges through a 22-year (2000–2021) historical series. Journal of Water and Health. Vol. 23, no. 6, pp. 671–83. June 1, 2025.
BATISTA, J. de S. et al. Intoxicações por alimentos e bebidas e ocorrência das doenças de transmissão hídrica e alimentar no Brasil. Saúde e Pesquisa. Vol. 15, no. 4, pp. 1–21. Dec. 7, 2022.
MARCYNUK, P. B. et al. Comparison of the burden of diarrhoeal illness among individuals with and without household cisterns in northeast Brazil. BMC Infectious Diseases. Vol. 13, 65. Feb. 4, 2013.
FERNANDES VIANA, G. G. et al. Assessing food safety practices and foodborne illness risk factors in Brazilian households. PLOS ONE. Vol. 20, no. 6, e0325070. June 18, 2025.
Republish
link








