Global burden of MDR-TB and XDR-TB: trends, inequities, and future implications for public health planning | BMC Infectious Diseases

Global
In 2021, the global ASIR of MDR-TB was 5.42 per 100,000 population (95% UI: 3.17, 9.34), with an ASMR of 1.28 (95% UI: 0.50, 2.53) and ASDR of 50.76 (95% UI: 21.28, 99.37). From 1990 to 2021, ASIR (AAPC = 0.14%, 95% CI: 0.13, 0.14), ASPR (AAPC = 0.21%, 95% CI: 0.20, 0.22), ASMR (AAPC = 0.03%, 95% CI: 0.02, 0.04), and ASDR (AAPC = 1.19%, 95% CI: 1.12, 1.26) all increased significantly (Table 1). In 2021, MDR-TB accounted for an estimated 0.44 million incident cases (95% UI: 0.26, 0.77), 0.65 million prevalent cases (95% UI: 0.38, 1.14), 0.11 million deaths (95% UI: 0.04, 0.21), and 4.13 million DALYs (95% UI: 1.71, 8.06), all showing upward trends (Supplementary Table S1).
For XDR-TB in 2021, the ASIR was 0.29 (95% UI: 0.21, 0.42), ASPR was 0.34 (95% UI: 0.23, 0.52), ASMR was 0.01 (95% UI: 0.00, 0.01), and ASDR was 3.47 (95% UI: 1.51, 6.43). From 1990 to 2021, significant increases were observed in ASIR (AAPC = 0.01%, 95% CI: 0.01, 0.02), ASPR (AAPC = 0.01%, 95% CI: 0.01, 0.02), ASMR (AAPC = 0.01%, 95% CI: 0.00, 0.01), and ASDR (AAPC = 0.11%, 95% CI: 0.11, 0.12) (Table 2). In 2021, XDR-TB was associated with 24,036 incident cases (95% UI: 17,144, 34,587), 27,933 prevalent cases (95% UI: 18,731, 43,751), 7,950 deaths (95% UI: 3,326, 14,859), and 287,736 DALYs (95% UI: 124,816, 531,852). All these indicators showed upward trajectories (Supplementary Table S2).
5 SDI regions
In 2021, the ASIR, ASPR, ASMR, and ASDR for MDR-TB were highest in low SDI regions and lowest in high SDI regions. Between 1990 and 2021, these indicators increased in low and low-middle SDI regions, while they declined in high SDI regions. Similarly, the number of incident cases, prevalent cases, deaths, and DALYs associated with MDR-TB rose across low-SDI, low-middle SDI, middle-SDI, and high-middle SDI regions (Table 1. Supplementary Table S1).
For XDR-TB, the ASIR and ASPR were highest in high-middle SDI regions, while the ASMR and ASDR were highest in low SDI regions, with the lowest values observed in high SDI regions. From 1990 to 2021, all indicators for XDR-TB increased across the five SDI regions (Table 2. Supplementary Table S2).
Geographic regions
In 2021, the ASIR was highest in Eastern Europe (16.73 per 100,000 population, 95% UI: 10.38, 24.72), ASPR in Southern Sub-Saharan Africa (21.31 per 100,000 population, 95% UI: 9.41, 44.94), ASMR in Eastern Sub-Saharan Africa (6.21 per 100,000 population, 95% UI: 2.40, 12.52), and ASDR in Eastern Sub-Saharan Africa (189.74 per 100,000 population, 95% UI: 75.50, 390.11). The ASIR declined in East Asia, High-income Asia Pacific, High-income North America, and the Caribbean, while it increased in 17 other regions, with the greatest increase observed in South Asia (AAPC = 0.49%, 95% CI: 0.47, 0.51). The ASPR decreased in East Asia, Central Europe, Australasia, High-income North America, and the Caribbean, but increased in 16 other regions, with the highest increase observed in South Asia (AAPC = 0.68%, 95% CI: 0.64, 0.71). The ASMR declined in East Asia, Central Europe, High-income Asia Pacific, Western Europe, Southern Latin America, High-income North America, and the Caribbean, while it increased in 11 regions, with the greatest increase observed in Eastern Sub-Saharan Africa (AAPC = 0.19%, 95% CI: 0.18, 0.20). The ASDR decreased in 8 regions, with the largest decline in East Asia (AAPC = −1.18%, 95% CI: −1.30, −1.05), and increased in 12 regions, with the greatest increase observed in Eastern Sub-Saharan Africa (AAPC = 5.93%, 95% CI: 5.64, 6.22) (Table 1). The number of incident cases of MDR-TB decreased in East Asia (AAPC = −234.50%, 95% CI: −323.18, −145.82) and High-income North America (AAPC = −7.74%, 95% CI: −7.87, −7.62), remained stable in High-income Asia Pacific (AAPC = −0.08%, 95% CI: −2.51, 2.36), and increased in all other regions (Supplementary Table S1).
In 2021, the ASIR of XDR-TB was highest in Oceania (0.64 per 100,000 population, 95% UI: 0.19, 1.49), while the ASPR (2.71 per 100,000 population, 95% UI: 1.80, 3.95), ASMR (0.56 per 100,000 population, 95% UI: 0.31, 0.90), and ASDR (24.86 per 100,000 population, 95% UI: 14.07, 39.55) were highest in Central Asia. From 1990 to 2021, the ASIR, ASPR, ASMR, and ASDR for XDR-TB increased across all 21 geographic regions, with the most significant increases observed in Central Asia (Table 2). Additionally, the number of incident cases, prevalent cases, deaths, and DALYs associated with XDR-TB also showed an upward trend in all 21 geographic regions (Supplementary Table S2).
204 countries and territories
In 2021, the ASIR of MDR-TB was highest in Somalia (57.25 per 100,000 population, 95%UI: 14.12, 169.56), as was the ASPR (66.95 per 100,000 population, 95%UI: 16.78, 191.63), ASMR (37.58 per 100,000 population, 95%UI: 7.63, 109.59), and ASDR (1066.78 per 100,000 population, 95%UI: 219.93, 3124.42) (Fig. 1A-D). From 1990 to 2021, the ASIR of MDR-TB increased in 155 countries, with the largest increase observed in Somalia (AAPC = 1.79%, 95%CI: 1.67, 1.92). It decreased in 40 countries, with the largest decline in Latvia (AAPC = −0.21%, 95%CI: −0.23, −0.19). The ASPR rose in 147 countries, with Somalia again seeing the largest increase (AAPC = 2.20%, 95%CI: 2.11, 2.28), while 44 countries experienced a decline, the greatest of which was in Latvia (AAPC = −0.31%, 95%CI: −0.36, −0.27). The ASMR increased in 120 countries, with the largest rise in Somalia (AAPC = 1.16%, 95%CI: 1.05, 1.27), while it decreased in 70 countries, with China seeing the largest reduction (AAPC = −0.04%, 95%CI: −0.04, −0.03). The ASDR increased in 120 countries, with Somalia showing the highest increase (AAPC = 37.62%, 95%CI: 34.13, 41.12), while 69 countries saw a decline, with China experiencing the largest drop (AAPC = −1.21%, 95%CI: −1.29, −1.12) (Fig. 1A-D. Supplementary Table S3 and S4).
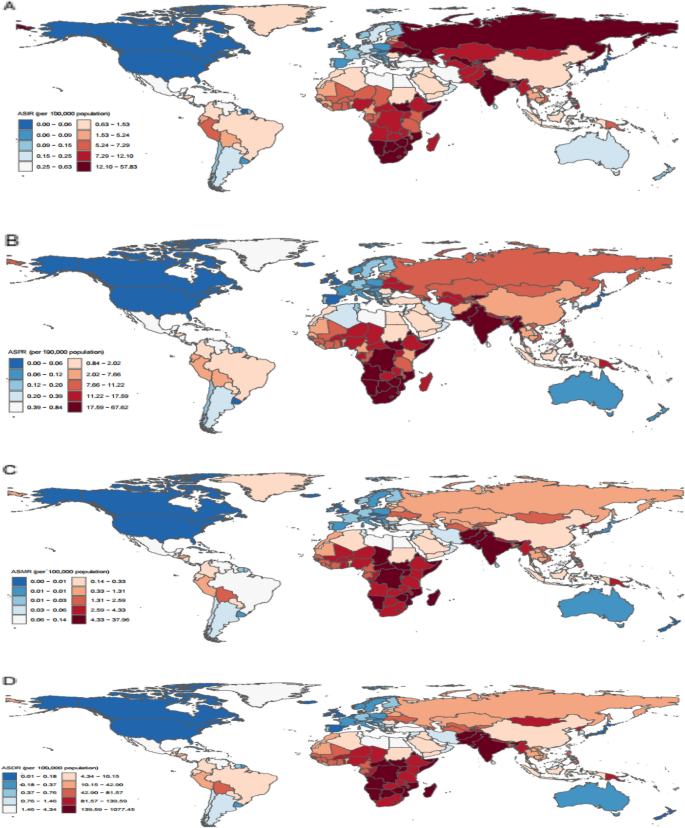
The global disease burden of MDR-TB in 204 countries and territories in 2021. A ASIR. B ASPR. C ASMR. D ASDR. Abbreviations: ASIR, Age-standardized incidence rate. ASPR, Age-standardized prevalence rate. ASMR, Age-standardized mortality rate. ASDR, Age-standardized disability-adjusted life years rate. DALYs, Disability-adjusted life years. MDR-TB, Multidrug-resistant TB without extensive drug resistance. TB, Tuberculosis
In 2021, India had the highest number of new cases of MDR-TB (0.22 million individuals, 95% UI: 0.05, 0.53), the highest number of prevalent cases (0.32 million individuals, 95% UI: 0.07, 0.77), the most deaths (0.05 million individuals, 95% UI: 0.01, 0.13), and the highest number of DALY cases (1.93 million individuals, 95% UI: 0.39, 4.79). Between 1990 and 2021, the number of new cases, prevalent cases, and DALYs all increased the most in India, while China experienced the greatest decreases (Supplementary Table S5 and S6).
In 2021, the ASIR of XDR-TB was highest in Kyrgyzstan (4.25 per 100,000 population, 95%UI: 1.41, 8.44), the ASPR was highest in Moldova (4.74 per 100,000 population, 95%UI: 2.79, 7.01), and the ASDR was highest in Mongolia (43.31 per 100,000 population, 95%UI: 9.55, 109.82) (Fig. 2A-D). Between 1990 and 2024, the ASIR, ASPR, ASMR, and ASDR of XDR-TB increased in all 204 countries and territories (Fig. 2A-D. Supplementary Table S7 and S8).
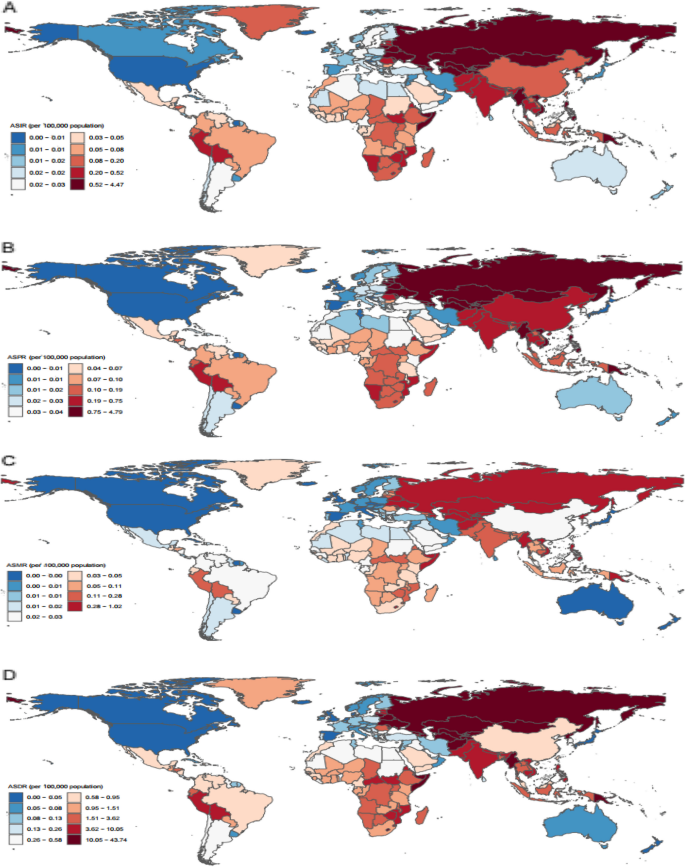
The global disease burden of XDR-TB in 204 countries and territories in 2021. A ASIR. B ASPR. C ASMR. D ASDR. Abbreviations: ASIR, Age-standardized incidence rate. ASPR, Age-standardized prevalence rate. ASMR, Age-standardized mortality rate. ASDR, Age-standardized disability-adjusted life years rate. DALYs, Disability-adjusted life years. TB, Tuberculosis. XDR-TB, Extensively drug-resistant TB
In 2021, the highest number of new cases of XDR-TB was in the Russian Federation (5,942 individuals, 95%UI: 3,172, 9,373), the highest number of prevalent cases was in India (7,512 individuals, 95%UI: 1,597, 18,276), the highest number of deaths was in India (2,815 individuals, 95%UI: 502, 7,178), and the highest number of DALY cases was in India (99,599 individuals, 95%UI: 17,968, 250,417). From 1990 to 2021, the number of new cases, prevalent cases, deaths, and DALYs due to XDR-TB increased in all 204 countries and territories (Supplementary Table S9 and S10).
Association between ASR and SDI
Between 1990 and 2021, significant inverse associations were observed between the SDI and ASRs for MDR-TB globally. Specifically, higher SDI levels were associated with lower ASRs for incidence (r = –0.50, P < 0.01), prevalence (r = –0.58, P < 0.01), mortality (r = –0.69, P < 0.01), and DALYs (r = –0.67, P < 0.01). Similarly, negative correlations were observed between SDI and the absolute numbers of incident cases (r = –0.33, P < 0.01), prevalent cases (r = –0.40, P < 0.01), deaths (r = –0.44, P < 0.01), and DALY counts (r = –0.49, P < 0.01) (Supplementary Fig. S1A-D. Table S11).
For XDR-TB during the same period, weaker yet statistically significant negative correlations were noted between SDI and ASRs: incidence (r = –0.09, P = 0.02), prevalence (r = –0.12, P < 0.01), mortality (r = –0.18, P < 0.01), and DALYs (r = –0.19, P < 0.01). However, associations between SDI and the absolute numbers of incident cases (r = –0.04, P = 0.02), prevalent cases (r = –0.04, P = 0.52), deaths (r = –0.04, P = 0.66), and DALY counts (r = –0.04, P = 0.08) were not statistically significant (Supplementary Fig. S2A-D. Table S11).
BAPC model prediction
By 2035, the ASIR of MDR-TB is projected to increase to 11.01 per 100,000 population (95%CI: 0.01, 23.98), while the ASMR is expected to rise to 2.47 per 100,000 population (95%CI: 0.01, 5.11). The ASIR of XDR-TB is projected to rise to 3.84 per 100,000 population (95%CI: 0.01, 23.52), and the ASMR to 1.34 per 100,000 population (95%CI: 0.01, 10.16). Between 2022 and 2035, the ASIR, ASPR, ASMR, and ASDR for both MDR-TB and XDR-TB are expected to show a declining trend (Table 3. Supplementary Fig. S3A-D, S4 A-D).
Decomposition analysis on DALYs cases
For MDR-TB, the global burden is predominantly driven by epidemiological changes (69.43%), with aging and population factors contributing 6.97% and 23.60%, respectively. High-middle and low-middle SDI regions show significant variations, with the high-middle SDI region experiencing a negative contribution from aging (−33.98%) and a large positive contribution from population change (122.84%). In contrast, the low-middle SDI region shows a large share from epidemiological change (71.20%) and a more balanced distribution across factors (Fig. 3A. Supplementary Table S12).
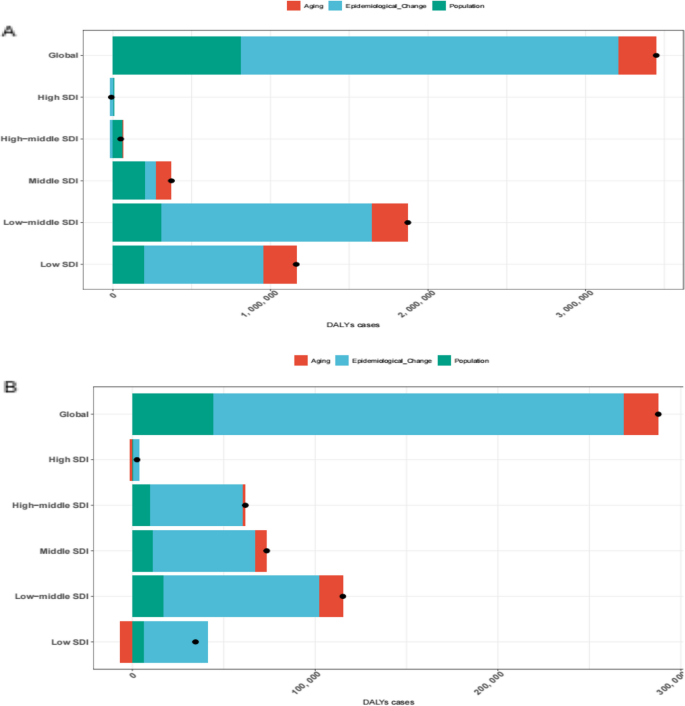
Impact of aging, population growth, and epidemiological changes on DALYs cases for MDR-TB and XDR-TB globally and across five SDI regions from 1990 to 2021 (A: MDR-TB. B XDR-TB). Black dots represent the total change in DALYs cases due to the combined effects of aging, population growth, and epidemiological shifts. Positive values indicate an increase in DALYs cases driven by the respective factor, while negative values indicate a net reduction in DALYs cases. Abbreviations: DALYs, disability-adjusted life-years. MDR-TB Multidrug-resistant TB without extensive drug resistance. SDI, sociodemographic index. TB, Tuberculosis. XDR-TB Extensively drug-resistant TB
For XDR-TB, the global burden is influenced heavily by epidemiological changes (100.87%), with negative contributions from aging (−19.44%) and minimal impact from population change (18.56%). High-middle SDI regions show positive contributions from population growth (15.41%) and aging (6.61%), while low SDI regions exhibit significant impact from epidemiological changes (132.79%) (Fig. 3B. Supplementary Table S12).
Cross-country inequality analysis for ASDR
For MDR-TB, the SII decreased from − 0.26 (95% CI: − 0.45, − 0.14) in 1990 to − 0.45 (95% CI: − 0.60, − 0.34) in 2021, indicating a widening absolute disparity, while the CCI exhibited a pronounced decline from − 12.15 (95% CI: − 14.03, − 10.27) to − 67.68 (95% CI: − 79.08, − 56.28), reflecting a substantial increase in relative inequality (Fig. 4A, B. Table S13). Similarly, XDR-TB demonstrated a marked expansion in inequality, with the SII decreasing from − 0.01 (95% CI: − 0.02, − 0.01) in 1992 to − 0.40 (95% CI: − 0.53, − 0.27) in 2021, and the CCI shifting from − 0.09 (95% CI: − 0.30, − 0.14) to − 0.24 (95% CI: − 0.38, − 0.08). These findings underscore a progressive concentration of both MDR-TB and XDR-TB burden among socioeconomically disadvantaged populations, highlighting the need for targeted public health interventions to mitigate growing disparities in drug-resistant TB (Fig. 4C, D. Supplementary Table S13).
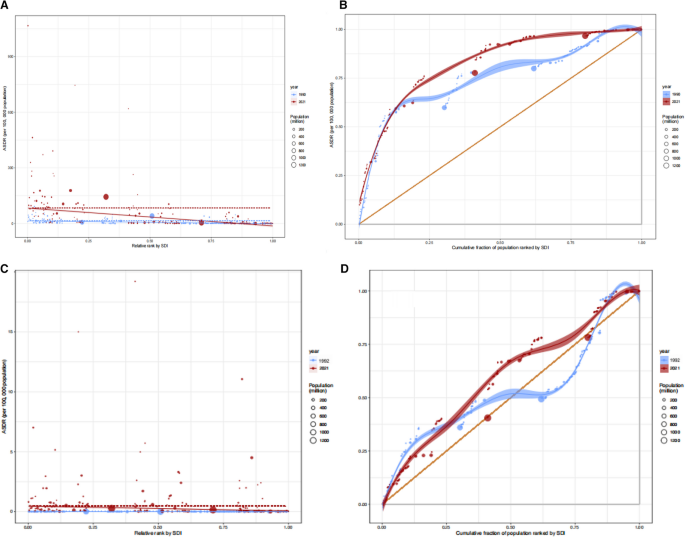
Regression and concentration curves illustrating health inequalities in the ASDR of MDR-TB and extensively XDR-TB across 204 countries and territories. Panels A and C present the SII for MDR-TB and XDR-TB, respectively. These panels depict the gradient of ASDR across countries, with data points scaled according to population size, thereby reflecting demographic weight. Panels B and D show the concentration curves, from which the CCI is derived. These curves illustrate the degree of relative inequality by comparing the cumulative ASDR distributions against cumulative population ranks stratified by SDI. Temporal shifts are color-coded: blue indicates baseline estimates (1990), while red denotes estimates for 2021. Abbreviations: ASDR, Age-Standardized disability-adjusted life-years rate. CCI, Concentration Index of Inequality. MDR-TB, Multidrug-resistant TB without extensive drug resistance. SDI, Sociodemographic Index. SI, Slope index of inequality. TB, Tuberculosis. XDR-TB, Extensively drug-resistant TB
Frontier analysis for ASDR
For MDR-TB, there was substantial potential for improvement, particularly in low- and middle-SDI countries such as Somalia, Lesotho, and South Sudan. Notably, several high-SDI regions, including Lithuania and Greenland, also exhibited considerable gaps in their ASDR levels (Fig. 5A, B. Table S14). Similarly, analysis of XDR-TB demonstrated considerable opportunities for ASDR reduction in countries across Central Asia and Eastern Europe, regions with moderate to high SDI. Countries like Kazakhstan, Ukraine, and Korea showed significant shortfalls in their expected performance, given their development levels (Fig. 5C, D. Supplementary Table S15).
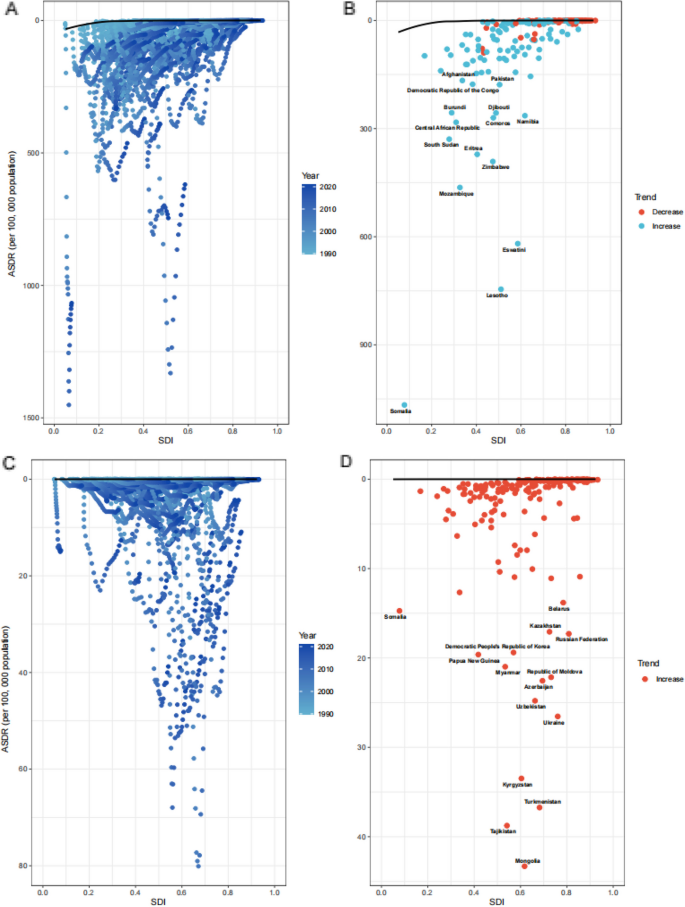
Frontier analysis examining the relationship between SDI and ASDR for MDR-TB and XDR-TB across 204 countries and territories. Panels A and C illustrate temporal shifts, where the gradient transition from Light to dark blue tracks the trajectory of national ASDRs in relation to changes in SDI from 1990 to 2021. Panels B and D present the ASDR cross-sectional distribution in 2021, with each point representing an individual country or territory. The black curve represents the estimated efficiency frontier, reflecting the lowest achievable ASDR for a given SDI level. Countries exhibiting the greatest deviations from the frontier are highlighted with labeled markers: red dots indicate high-SDI countries that are underperforming, while Light blue dots denote low-SDI countries that are positioned closer to the frontier. The change in ASDR between 1990 and 2021 is color-coded, with orange indicating a net decline and light blue denoting a net increase. Abbreviations: ASDR, Age-Standardized disability-adjusted life-years rate. MDR-TB, Multidrug-resistant TB without extensive drug resistance. SDI, Sociodemographic Index. TB, Tuberculosis. XDR-TB, Extensively drug-resistant TB
link





